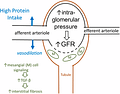
High dietary protein intake and renal health
One of the inevitabilities of aging seems to be a progressive degradation of kidney function as measured by the estimated glomerular filtration rate (eGFR), independent of underlying disease.1 Increased blood pressure and poor glucose homeostasis, more common with increasing age, are strongly associated with more rapid deterioration of kidney function.2 Still, even healthy individuals will start to witness their kidney function decline from the third decade of life onwards.3
There are many proposed mechanisms behind this progressive degradation of renal health.4 Not only does chronic high blood pressure and subsequent endothelial dysfunction and microvascular damage cause nephrosclerosis, i.e. hardening of the arterial and arteriolar walls in the nephron but even repeated short bouts of increased blood pressure are proposed to cause accumulating damage over time. Chronic hyperglycemia and accumulated advanced glycation end products (AGEs), as observed in diabetic populations, are also thought to be causal factors contributing to the progressive worsening of renal function.5 Similarily to transient hypertension, acute hyperglycemia has been proposed as a contributing factor to renal injury.6 It’s conceivable that this would, over long periods of time, drive the progressive worsening of kidney function with age, especially in the current food environment where acute hyperglycemia, even in the absence of chronically elevated glucose levels, is prevalent.
There are of course many other things beyond hypertension and hyperglycemia that contribute to age-related worsening of kidney function: acute kidney failure, dehydration, use of nephrotoxic compounds, infections, increased volume loads, increased intra-abdominal pressure, comorbidities, and so on.7 With the increased awareness of the benefits of high-normal dietary protein intakes, concern over possible harmful effects on the kidneys has emerged. The basis for this concern is twofold. Firstly, as Martin et. al. puts it:
At the center of the controversy is the concern that habitual consumption of dietary protein in excess of recommended amounts promotes chronic renal disease through increased glomerular pressure and hyperfiltration. Media releases often conclude that, "too much protein stresses the kidney".8
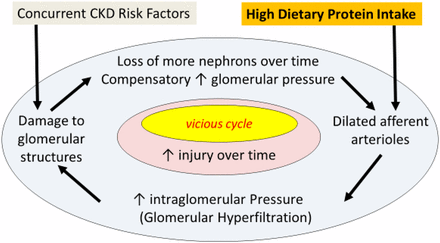
Secondly, as concluded in The Effects of High-Protein Diets on Kidney Health and Longevity by Gang-Jee et al.:
Although high-protein diets continue to be popular for weight loss and type 2 diabetes, evidence suggests that worsening renal function may occur in individuals with—and perhaps without—impaired kidney function. High dietary protein intake can cause intraglomerular hypertension, which may result in kidney hyperfiltration, glomerular injury, and proteinuria.9
Low protein diets reduces nitrogen waste products and decrease kidney workload by lowering intraglomerular pressure, which may protect the kidneys especially in patients with decreased nephron capital and renal function. It leads to favorable metabolic effects that can preserve kidney function and control of uremic symptoms…10
Furthermore, there seems to be some evidence to suggest that protein restriction in presence of chronic kidney disease (CKD) will slow disease progression:
Population-level data indicate graded risk for progressive renal functional decline with increasing protein intake among women with mild renal insufficiency, and support a possible association of higher protein consumption with the risk of microalbuminaruia in people with concomitant diabetes and hypertension. A link between the quantity of protein intake and the rate of renal deterioration is suggested by preliminary prospective studies among incident peritoneal dialysis patients, renal transplant recipients, and animal models of kidney disease.11
Also, from the previously mentioned paper by Martin et. al.:
Observational data from epidemiological studies provide evidence that dietary protein intake may be related to the progression of renal disease. In the Nurses' Health Study, protein intake, assessed with a semi-quantitative food frequency questionnaire, was compared to the change in estimated GFR over an 11-year span in individuals with pre-existing renal disease. Regression analysis showed an association between increased consumption of animal protein and a decline in renal function suggesting that high total protein intake may accelerate renal disease leading to a progressive loss of renal capacity.
In my post Exercise Framework, I elaborate on why muscle mass and strength are cornerstones of health and can protect us from death. Progressive loss of muscle mass is an inevitable part of aging and dietary protein plays a crucial role in maintaining healthy amounts of muscle. In their recent paper, Aragon et. al. make a case for why consuming dietary protein beyond the RDA12 is beneficial:
Age-related muscle anabolic resistance may be overcome, and sarcopenia progression offset, by maximizing postprandial MPS through structured resistance training. A large meta-analysis by Morton et al (49 randomized controlled trials, 1863 subjects) concluded that a protein intake of approximately 1.6 g/kg/day (with an upper 95% confidence interval of 2.2 g/kg/day) maximizes resistance training–induced muscle hypertrophy and strength gains in adults under eucaloric or hypercaloric conditions. However, it was also found that gains in fat-free mass were reduced with increasing age. This calls into question the effectiveness, and possibly the sufficiency, of the 1.6 g/kg/day benchmark when applied to older adults. It is therefore possible that this intake level should be the minimum to be maintained through older age, alongside regular resistance-type exercise, if the goal is to maximize sensitivity to anabolic stimuli and preserve muscle mass.
The authors go on to state that:
It was clear that protein intakes of ≥1.6 g/kg show muscle size and strength gains in subjects under the age of 65 years, but there is also a clear lack of data on such intakes in subjects who are 65 years and beyond. Furthermore, there is an absence of trials directly comparing 1.6 g/kg with higher intakes, so the commonly presumed optimality of this dose is still speculative—especially in older adults.13
The question that arises from these conclusions, namely from the claim that a high-protein diet in healthy individuals is causing a progressive decrease in kidney function and from the claims on the importance of protein for optimizing muscle is if high dietary protein consumption really is causing damage to the kidneys and subsequent increased risk for CKD. In theory, at least, we’d like to discover an optimal range where we consume an adequate amount of protein to maximize muscle growth and retention as we age, and at the same time make sure to preserve our renal function at least as good or even better than the top percentiles of our age cohort.
Let’s elaborate a bit on this age cohort point. If we’d like to live, let’s say, two decades longer than the average life expectancy (i.e. to a hundred or so), our renal function should be better than the median renal function of someone two decades older than us. The numbers might not be quite right here, but the point is that we cannot settle for average eGFR at any point in our life, since the projected deterioration will ultimately wipe us out if nothing else does earlier. This holds of course true for most biomarkers with predictive value: average glucose, apoB, VO2 max, and the list goes on.
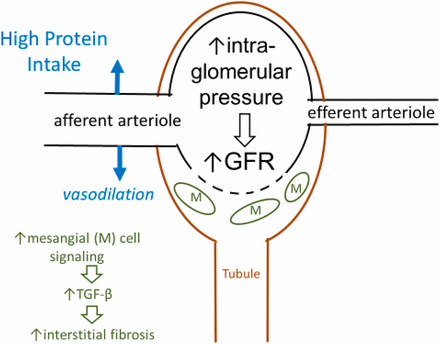
So is there actually any convincing evidence that high dietary protein intake in healthy people (i.e. people without kidney disease) would be harmful? As mentioned earlier, the proposed mechanism is one where high dietary protein intake results in increased glomerular pressure and hyperfiltration. Thomas et. al. explain in their paper What does the renal reserve mean? that it’s quite likely that the main mechanism by which a significant increase in eGFR can be observed when consuming high amounts of protein is due to renal vasodilation, allowing larger blood volumes into the nephron, increasing the flow, and hence increasing the pressure in the glomeruli and with which solutes filter out. It’s this increase in intra-glomerular pressure that is thought to be harmful to renal health in the long run. In fact, mechanistic evidence on angiotensin receptor blockers (ARBs), the first-in-line blood pressure medications with meaningful kidney protective properties, has demonstrated that decreasing intra-glomerular pressure by dilating mainly but not exclusively the efferent arteriole is profoundly kidney protective.1415 Thus we might think that increasing intra-glomerular pressure is harmful to the kidneys, but extrapolating like this from mechanistic data is far from convincing evidence.
Before getting into the studies looking at dietary protein intake and renal health, we should address a major issue with observational studies. As quoted earlier from a paper by Martin et. al.:
Observational data from epidemiological studies provide evidence that dietary protein intake may be related to the progression of renal disease. In the Nurses' Health Study, protein intake, assessed with a semi-quantitative food frequency questionnaire, was compared to the change in estimated GFR over an 11-year span in individuals with pre-existing renal disease. Regression analysis showed an association between increased consumption of animal protein and a decline in renal function suggesting that high total protein intake may accelerate renal disease leading to a progressive loss of renal capacity.
Even though 11 years would conceivably be a long enough time period to see some deterioration in kidney function if there was some to be observed, the data on which the conclusions are made should be questioned. Firstly, food frequency questionnaires are not reliable sources of information on dietary intake. Secondly, we have no idea what the background diet of those consuming higher protein looks like. I’d actually argue that it’s highly likely that people who consume higher amounts of protein do also consume more fat, salt, and calories. You see, most protein-rich foods are also quite high in fat (beef, eggs, dairy, sausages), and/or prepared in a way that makes the protein source less “clean” (breading, frying, adding a lot of salt, processing meat), and/or eaten in a combination that is calorically dense and easy to overeat. Most people are not consuming their protein in form of lean meats or low-fat dairy, legumes, and fish, but rather in combination with a lot of carbohydrates and from sources containing a lot of fat and salt. Lastly, we cannot infer causality from observational data. An association between higher protein intakes and worse renal function does not mean that either one causes the other.
The trend nowadays is for people to be more cognizant of their diets. A tendency to focus on leaner protein sources with a background diet that is nutrient-rich and high in fiber is observable, and it’s these kinds of diets’ impact on renal health that should be studied.
Even though no single paper that would tie the evidence together conclusively has been written on the subject of dietary protein intake and renal health, different bits and pieces can be investigated to gain confidence in our primers. I will again mention the paper Dietary protein intake and renal function by Martin et. al. which states:
Although the efficacy of high protein diets for weight loss has been evaluated, there have been no reports of protein-induced diminutions in renal function despite subject populations that are generally at risk for kidney disease (e.g., dyslipidemia, obesity, hypertension)
The authors go on to cite a paper where:
…65 overweight, but otherwise healthy, subjects adhered to a low or high protein diet for six months. In the high protein group, both kidney size and GFR were significantly increased from that measured at baseline. No changes in albumin excretion were noted for either group and the authors concluded that, despite acute changes in renal function and size, high protein intake did not have detrimental effects on renal function in healthy individuals.
… and conclude from a shorter-term study that:
No significant changes were noted in serum or urinary creatinine and albumin excretion, suggesting no ill-effects of a high protein diet on renal function.
Furthermore:
Poortsmans and Dellalieux found that protein intakes in the range of ~1.4–1.9 g/kg/day or 170–243% of the recommended dietary allowance did not impair renal function in a group of 37 athletes. We found no data in the scientific literature to link high protein intakes to increased risk for impaired kidney function in healthy, physically active men and women.
Even higher amounts than Poortsmans and Dellalieux have been used by Antonio et. al. in a cross-over study in resistance-trained men. The study had the subjects eat their “normal” diet (2.51g +- 0.69g of protein per day) and then crossed them over to increase their protein intake to 3.32g +- 0.87g per day. The authors conclude from their study that:
…we found no deleterious effects of a high protein diet (2.51–3.32 g/kg/d) over a 1-year period. Prior work from our lab has shown that consuming a high protein diet in the short term has no harmful effects on any clinical measure (i.e., blood lipids and comprehensive metabolic panel).
In male subjects with several years of experience with resistance training, chronic consumption of a diet high in protein had no harmful effects on any measures of health. Furthermore, there was no change in body weight, fat mass, or lean body mass despite eating more total calories and protein. Contrary to popular belief, the consumption of a high protein diet is not mutually exclusive with a diet high in fiber nor does the consumption of cholesterol above the standard recommendations result in any untoward effects on blood lipids. This is the first 1-year longitudinal investigation in resistance-trained males that demonstrates the lack of harm caused by a high protein diet.16

A systematic review and meta-analysis by Schwingshackl and Hoffmann looked at 30 studies including 2160 subjects without CKD to determine the effects of high-protein intakes on parameters of renal and metabolic health.17 The authors did only include studies looking at post-intervention results, meaning that the study participants were not compared to themselves before the intervention. Rather, participants in the high-protein groups were compared to participants in the normal-/low-protein groups. Measured outcomes might, and likely did vary before the studies were conducted, which makes conservative interpretation advisable.
Reviews like this are in many ways problematic. Firstly, pooling together a bunch of studies that claim to have used high-protein intakes can be misleading due to there not being any standardized definition for high-protein intakes. Some studies define high-protein as above the RDA, others as >2x above the RDA, and so on. Secondly, it’s not clear that the outcomes measured by the individual studies in the meta-analysis are comparable. Renal function can be measured with many biomarkers with variable assays, and these might not be interchangeable when assessing effects. Lastly, we should be careful when drawing conclusions from population-level data to the individual. It’s not clear that the populations in the individual studies are comparable in terms of their response to higher protein intakes. Furthermore, it’s important to recognize the limitations that the duration of the individual studies proposes for the meta-analysis. Schwingshackl and Hoffmann included studies with intervention periods of one to 108 weeks, of which the former is certainly too short of a time to observe any meaningful impacts (i.e. higher risk of chronic renal disease). It’s not clear how long we should follow up on people with high dietary protein intakes to be able to make any meaningful conclusions. Natural experiments are ongoing and seem to point in the direction of protein not being in and of itself nephrotoxic.
A major limitation of nutritional intervention trials is the heterogeneity of various aspects and characteristics of the study protocols. Therefore, it is not surprising that the RCTs and crossover studies included in the present analyses varied regarding type(s) of diets used (energy restriction, isocaloric), definitions of HP and NP/LP diets, study population (i.e. age, sex, healthy, overweight, obese, type 2 diabetics), intervention time (1–108 weeks), as well as nutritional assessment.
Nevertheless, Schwingshackl and Hoffmann conclude:
Changes in serum creatinine, urinary albumin excretion, uric acid, and urinary pH were not significantly different following HP diets as compared to NP/LP diets…
HP diets were associated with a significantly more pronounced increase in GFR as compared to NP/LP protocols
Serum urea and urinary calcium excretion were significantly more increased by HP diets in comparison to the NP/LP settings

As we can observe from the figure above, a significant portion of the variance in the results, especially with regard to serum urea, urinary calcium excretion, and urinary pH, is attributable to study heterogeneity, i.e. to the "difference in the [individual] studies themselves, the investigated populations, treatment schedules, endpoint definitions, or other clinical diversity."18
The authors summarize the results as follows:
The main findings suggest that subjects following an HP diet presented themselves with increased GFR, serum urea, and urinary calcium excretion, respectively. Further increases in serum concentrations of uric acid could be observed in those individuals following an HP regimen, when the trial by Jenkins et al. (2001) was excluded from the analysis due to the fact, that it was the only study using vegetable protein exclusively as a supplement.
I’ve written about uric acid (UA) previously, and it’s clear that higher protein intake (and especially purine intake from animal sources) can contribute to increases in serum uric acid levels. I personally think UA is one of the biomarkers to regularly follow up on, and interventions to lower UA should be conducted if needed. This doesn’t imply that one should shy away from higher protein diets due to possible increases in UA, as the benefits quite certainly overweigh the negatives.
Creatinine, even though far from perfect, is the major biomarker that is used to calculate eGFR. Schwingshackl and Hoffmann did not observe an increase in creatinine with higher protein intakes, indicating no ill effects on renal function. Furthermore, urinary albumin excretion, a measure often elevated in nephrotic syndrome indicating renal damage, did not increase. Conservative interpretation is advised for both of these measures as the p-values of the results leave room for improvement.
In summary, I don’t think there’s any convincing evidence to suggest that high dietary protein intake would be harmful to renal health acutely or in the long run in individuals with healthy renal function. This should be distinguished from the possibility that low dietary protein intake might be protective of renal health in the long run, something I did not touch on here. Although disputed1920, there’s also some evidence suggesting that lower protein intake in patience with CKD might improve prognoses.2122 This, however, should not be interpreted to mean anything in "healthy" individuals. Moreover, what I didn't touch on in any significant way here is the benefits of higher dietary protein intake (vs. the RDA). The effects on body composition, metabolic health, and blood pressure are significant and should not be overlooked, and it might be the case that the benefit gained from optimizing these with the help of higher dietary protein intakes far outweighs the negatives.
As is the case with every attempt to look at how dietary factors influence health outcomes in the real world, we're ultimately limited by our own tools. Everyone should establish, by means of consistent methods, a level of confidence in the evidence at hand that allows them to draw practical conclusions applicable to the real world. In light of new information, the level of confidence in the evidence should be adjusted, and the expectations and practical strategies updated, accordingly.
“For example, the ESPEN Expert Group recommends a protein intake of at least 1.0 g/kg/day–1.2 g/kg/day for healthy older people, 1.2 g/kg/day–1.5 g/kg/day for older people who are malnourished or have an acute or chronic illness, and even higher intakes for individuals with severe illness or injury. The PROT-AGE Study Group recommends an average daily intake of 1.0 g/kg/day–1.2 g/kg/day for healthy individuals, 1.2 g/kg/day–1.5 g/kg/day for those with an acute or chronic disease, and up to 2.0 g/kg/day for those with malnutrition, severe illness, or injury.” (13)