I’ve for a long time been interested in the health impacts of electrolytes, and how to optimize intake for performance and longevity. I’ve personally always salted my food quite liberally. This is partly due to preference and partly because I exercise a lot and use the sauna regularly = I sweat a lot. I’m prone to hypotension (mainly due to genetics I’d guess) and have quite a taste for salty food, an indicator of insufficient sodium status (and certainly preference as well, since I much more prefer salt over sweet). Moreover, I’ve had bouts of orthostasis and mild postural hypotension, indicating some sort of electrolyte insufficiency. All of this has led me to become quite interested in electrolyte balance, and I’ve already talked about the importance of magnesium when it comes to calcium homeostasis. Here I’m going to talk a bit about sodium, and the surprisingly notable dogma and ignorance that the mainstream medical establishment maintains toward sodium.
By the way, “salt” is used interchangeably with sodium. Salt, meaning table salt, is sodium chloride (NaCl) and contains 39.34% sodium. Sodium can be attained from NaCl, but also from, for example, MSG (monosodium glutamate). Sodium is what we are talking about here, but it’s important to realize that this is basically the same thing as salt, at least in the context of this discussion.
During our course on cardiovascular physiology and nephrology, we discussed blood pressure (BP) regulation extensively. I’ve written about the importance of having near-optimal blood pressure, and am still of the opinion that BP is the most important cardiovascular metric to optimize for. It’s unquestionable that sodium plays a critical role in the maintenance of normovolemia (normal blood volume), and thus blood pressure. Sodium suspended in water causes increased osmolality of the solution. This means that water will “flow” to places where sodium concentrations are higher, to balance out the sodium concentration between areas of high and low osmolality in a solution. Another way of putting this is that sodium attracts water. Following this logic, it would make sense that increases in sodium intake, and thus sodium concentrations of the blood, would increase blood volume and drive BP up. Following this logic is also ignorant and quite frankly stupid. Simplifying physiology to a single variable is not acceptable.
There’s clearly more to this blood pressure picture: a more complicated homeostatic mechanism behind blood pressure regulation. Homeostatic in the sense that low BP will cause a system responsible for highering BP to kick in, and vice versa. Just look up the RAA-system, vasopressin, Kinin–kallikrein system, and atrial natriuretic peptide. Before summarizing these, let’s give a primer on hydration: hydration is mainly driven by sodium and potassium (and glucose, creatine, and other molecules to some extent). Simply put: sodium will hydrate the outside of the cells (blood circulation, extracellular space, etc…) and potassium will hydrate the inside of the cells (muscles, and so on). For sodium and potassium to be in the right place, the sodium-potassium pumps need to pump potassium into the cell and sodium out of the cell. This requires energy. Energy status is mainly dictated by metabolic and mitochondrial health. This is an extremely simplified picture I give here, but it will do for now. The most important takeaway is that sodium drives hydration outside of the cells and potassium inside of the cells. Moreover, we need to remember that water is the “substrate” for hydration. Without water, there’s no hydration. Water follows sodium and potassium, and energy establishes the right place and concentrations for these electrolytes. With too low sodium concentrations (hyponatremia), the outside of the cell will become “dehydrated”, and the same holds for the inside of the in a state of hypokalemia.
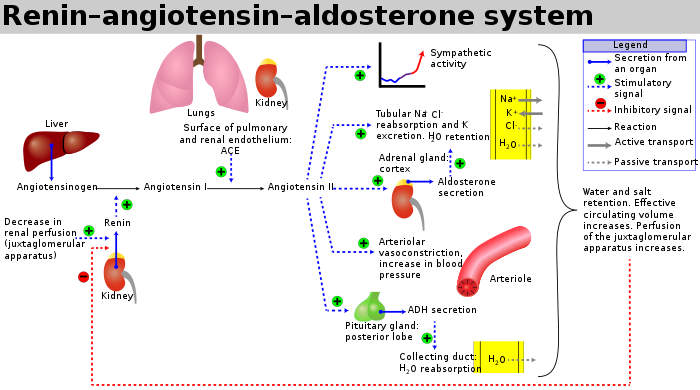
Ok, then, so here’s the summary: RAAS (renin-angiotensin-aldosterone system)kicks in when blood pressure is low i.e. when blood osmolality is low, or when blood volume is low. The kidneys will detect the low BP and secrete renin. Renin will cleave angiotensinogen, produced by the liver, into angiotensin I. Angiotensin I will be converted into the active hormone angiotensin II by ACE (angiotensin-converting enzyme) mainly in the lungs, endothelium, kidneys, and the brain. Angiotensin II causes potent vasoconstriction by binding to the AT-1, thus raising blood pressure. Angiotensin II will also promote the secretion of aldosterone, a mineralocorticoid responsible for further increasing BP. Further, angiotensinogen II is stimulating the secretion of vasopressin (ADH, antidiuretic hormone), causing the kidneys to hold on to more water, thus increasing plasma volume and BP.
The RAAS is mainly responsible for the maintenance of normotension and normovolemia. BP is crucial for the oxygenation of tissues, especially the brain. In cases of hypovolemia, ex. loss of blood, the RAAS kicks in at full gear. It’s proposed that overactive RAAS would be the underlying cause of increased hypertension rates, mainly due to the longevity-promoting effects of AT-1 antagonists (ARB, angiotensin receptor blockers) in people with chronic diseases (CKD, CHF, etc…). Further, ARBs seem to have pleiotropic effects on the PPAR enzymes and thus modulate metabolism more broadly. (Ref. from my med. notes below)
There are some systems responsible for vasodilation as well (lowering BP). Vasodilation is important for the innate immune response, and vasodilation is often seen in cases of allergies or anaphylaxis. These effects seem to be mediated partially by the Kinin–kallikrein system, as well as secretions from leukocytes. Atrial natriuretic peptide (ANP) causes decreases in extracellular fluid volume by increasing the secretion of sodium. As mentioned before, sodium is the main driver of extracellular hydration. ANP is secreted from the heart in response to high blood volume, and increases renal sodium excretion (ie you’ll pee out more sodium). There’s more than this to blood pressure, but I won’t bore you further with all this physiology. Let’s talk about some epidemiology and practical stuff.
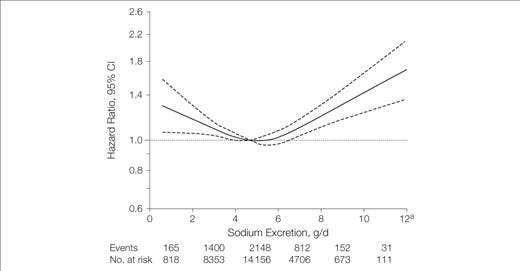
There’s this one, often-referenced picture, showing how urinary sodium excretion is associated with mortality.
As we can clearly observe from the figure, the association between urinary sodium excretion (the amount of sodium one is peeing out) and mortality is U-shaped, as happens to be the case with almost any variable and mortality (not to shit on this observation in any way). I’d think that sodium excretion is a good proxy for intake, since once homeostasis is reached, there shouldn’t be any meaningful net difference in intake and excretion (if we assume sodium loss from sweating and stuff to be near zero, which is not the case in athletes, but the cohorts here are not athletes). So I’m going to use excreted sodium as a proxy for intake, like everyone else looking at this study. Increasing sodium intake from 0 grams to around 5 grams a day (that’s btw something like 11 grams of salt) yields longevity benefits. Going higher than 6 grams seems to be counter-productive. Chriss Kresser writes in his post on salt: “not only was lower sodium excretion associated with higher CVD mortality, but baseline sodium excretion did not predict the incidence of hypertension, and any associations between systolic pressure and sodium excretion did not translate into less morbidity or improved survival”, referencing the same material. You can read the full post by Kresser here. It’s important to understand here that the medical recommendation for lowering BP and maintaining a healthy BP, is to limit sodium intake. In a lecture given to us in medical school, there was a reference to observational studies done on hunter-gatherer tribes. These consume naturally low amounts of sodium and have almost no hypertension. This is used as an argument in favor of low-salt diets. But what about the extreme amounts of cardiovascular output, the relative to western populations’ extremely high potassium and magnesium intake, and the non-existence of overweight and obese individuals, hyperglycemic foods, and of hyperinsulinemia? The simplified views that we students on the university level have to endure are comical, to say the least…
I might sound antagonistic toward the anti-sodium arguments, but trust me, I’m not. I just think sodium is an overstated part of this complex situation and further investigation is required. Giving general recommendations (lower your salt intake) in a situation as complex as this one is just crazy to me. We need more sophisticated tools based on individual responses and need to avoid these overly simplified, 0th-order views on things.
Let’s finish off with a few words on potassium and some general thoughts on how to approach this stuff. There have been some issues with the studies investigating optimal sodium and potassium intake. Firstly, it’s clear that some people are “salt-sensitive”, i.e. these people do not excrete sodium quite as effectively in response to rising blood sodium concentrations as “non-salt-sensitive” people do. This results in increased blood pressure in response to higher sodium intake. This hints at how the body normally reacts to high sodium concentrations (in response to intake): one is peeing out the sodium. There’s only one caveat, namely that one needs potassium for sodium to get excreted. The recommended intake of potassium is 5 grams, and almost no one hits that (compared to hunter-gatherer intake of about 12 grams, as I mentioned earlier). In the case of insufficient potassium intake, sodium can’t get excreted effectively and is going to drive increased plasma osmolality. Nowadays people consume fewer foods high in potassium such as fruits, vegetables (not boiled), nuts, legumes, and meat. Grains and rice, dairy, and processed foods are devoid of potassium.

Here we need to realize one thing. The institutions responsible for establishing the recommended daily intakes (RDIs) and daily adequate intakes (AI) have aggressively moved towards evidence-based standards, and make their decisions mainly based on randomized controller trials (RCTs) and large meta-analyses. This is all great, we all want the studies to be rigorous and well done. The institutions have established an upper limit for a sodium intake of 2300 mg (US) and 5g of salt per day (around 2000g sodium, Fin). For potassium, the adequate intakes are around 1600-2000mg (US) and 3000-3500mg (Fin) but note that these are adequate intakes, not recommended intake, which is around 5000mg. There’s also another metric put into place for sodium, but not for potassium. Namely, Chronic Disease Risk Reduction level (CDRR). This is the amount of sodium that should be consumed (or not consumed) for one to avoid the risk of chronic disease. But why has it been established for sodium and not potassium? Establishing the CDRR requires studies that are powered to find and investigate impacts on chronic health outcomes, such as mortality or adverse events. For sodium there specifically exists RCTs that look at these. In the case of potassium, the trials have only looked at blood pressure outcomes (potassium lowers blood pressure), but not at chronic disease outcomes or clinical end-points. This means that the studies on potassium are not “evidence-based”-enough, and/or do not investigate the right outcome for them to be used for establishing guidelines (this is because the studies were done before the boom of evidence-based medicine and hierarchy or evidence and study design) and are thus dismissed completely, even though potassium clearly lowers blood pressure. A change in study design and wording would make the potassium trials eligible for establishing CDRR (if the studies would have measured the impact on cases of hypertension instead of the impact on blood pressure). The obvious and strong interplay between sodium and potassium makes a case for establishing this. All of this anti-salt talk has led us to only concentrate on one piece of the puzzle, all the way through the system, from individual physicians to institutions at large. Moreover, this is a shortcoming of the evidence-based narrative and practically shows why the ability to interpret studies is so important in today’s scientific milieu.
It’s clear that blood pressure is more complicated than we are led to believe, even at the level of medical school. The practical takeaway is that one should monitor one’s BP, and if it’s high, increase potassium intake slowly. One can also start by lowering sodium intake in case of high intakes. Adequate intake of magnesium is also important (around 400mg-800mg of elemental magnesium per day). Lowering glycemic load, eating whole foods and limiting alcohol and smoking, having a structured exercise routine of both resistance and aerobic exercise, and so on, are all going to support healthy blood pressure regulation.
By the way, I’m not a medical doctor, and this is not medical advice. You should absolutely reach out for medical attention if you have any issues with your blood pressure. There are many reasons for this beyond any dietary or lifestyle factor, some of which require immediate care.